What does it actually take to catch a neurological decline before it becomes irreversible?
For most hospitals, the answer still involves a penlight, a trained eye, and a clinician's best judgment. That approach has worked for decades, but it has real limits. Subjectivity creeps in. Documentation varies by shift. And in high-acuity settings, inconsistency costs time that patients don't have.
The Documentation Problem Nobody Talks About
Ask any ICU nurse how two colleagues might describe the same pupil response, and the answers won't always match. Neither is wrong, but those small differences in a neuro exam create noise in a patient's chart that makes trend-tracking genuinely difficult. That inconsistency isn't a training failure. It's a structural one. And it's exactly where purpose-built neurological tools are making a measurable difference.

From Estimation to Standardized Measurement
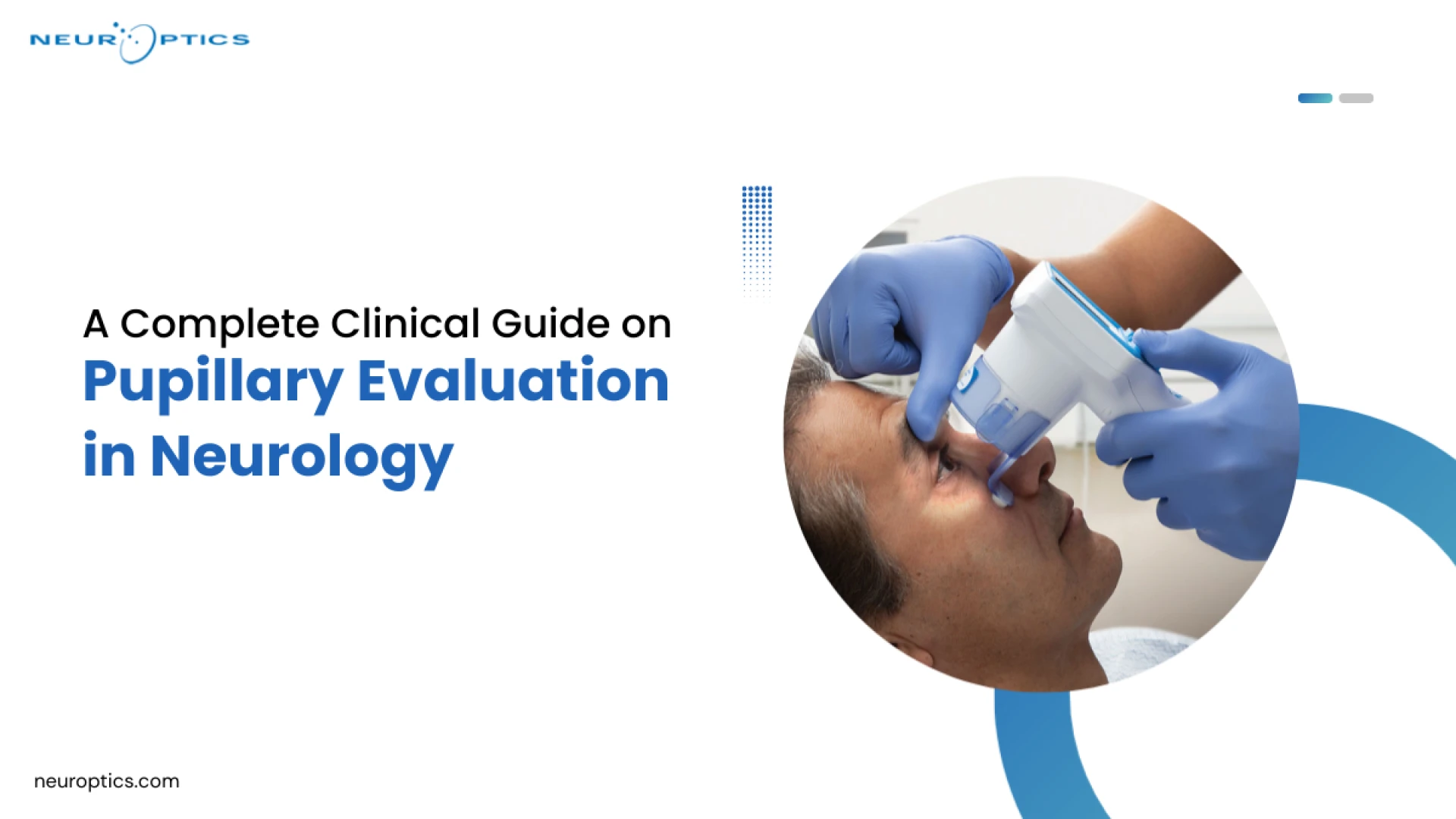
Automated pupillometry, particularly devices that generate an Npi pupillometer score, removes the guesswork. Instead of estimating reactivity, clinicians receive a standardized number - one that holds the same meaning regardless of who's running the assessment or what shift it is.
| Assessment Factor | Manual Method | Automated with NPi |
| Measurement basis | Clinical estimation | Quantitative scoring |
| Cross-shift consistency | Variable | Standardized |
| Trend tracking | Chart-dependent | Continuous, comparable |
| Early decline detection | Experience-driven | Threshold-based alerts |
Hospitals that have adopted this approach report that their teams spend less time debating documentation and more time acting on it.
Real Clinical and Operational Impact
Earlier detection of intracranial pressure changes translates directly into faster intervention windows. That matters clinically, and it matters financially. Shorter ICU stays, fewer avoidable escalations, and cleaner audit trails all follow from a more reliable neuro exam workflow. Most platforms also integrate with existing EHR systems, so implementation doesn't require rebuilding processes from scratch. Piloting in one high-acuity unit before a facility-wide rollout has worked well for institutions looking to manage adoption carefully.
FAQs
Q: Are these tools appropriate across all patient types?
A: Current validation is strongest in adult ICU, neurology, and post-surgical settings. Device guidelines should be reviewed for pediatric applications.
Q: Does NPi pupilometer scoring replace clinical judgment?
A: No. It supports it. The score flags changes that warrant a closer look, but the clinician still makes the call.
Q: What does ROI look like for hospitals?
A: Fewer preventable escalations and stronger documentation for compliance audits are the most consistent financial benefits reported.
Final Thoughts
Neurological care doesn't need to be reinvented; it needs better inputs. Standardized, objective data give clinical teams something reliable to work with, and that reliability compounds over time into better outcomes and more defensible care decisions.
Contact NeurOptics today to find out how smarter pupillary evaluation assessment tools can strengthen neurological care across your facility.







Sign in to leave a comment.