Charcot neuroarthropathy is a debilitating condition that exemplifies the complex relationship between nerve damage and joint destruction. Often associated with diabetes, this condition can lead to severe deformities and complications in the feet and ankles, significantly affecting an individual’s quality of life. Understanding the underlying mechanisms, risk factors, and management strategies for Charcot neuroarthropathy is crucial for both patients and healthcare providers. This article explores the intricacies of this condition, shedding light on its causes and implications while emphasizing the importance of early intervention and appropriate treatment.
Understanding Charcot Neuroarthropathy
Charcot neuroarthropathy is characterized by the progressive degeneration of joints, most commonly in the foot and ankle, due to a loss of sensory innervation. The condition typically occurs in individuals who have experienced peripheral neuropathy, a condition that impairs the nerves responsible for sensation in the extremities. When the nerves are damaged, individuals may lose the ability to feel pain, pressure, or temperature changes in their feet. This loss of sensation can result in unrecognized injuries, leading to repetitive trauma and, ultimately, joint destruction.
The history of Charcot neuroarthropathy dates back to the late 19th century when it was first described by the French neurologist Jean-Martin Charcot. Initially associated primarily with tabes dorsalis, a complication of syphilis that affects the spinal cord, the condition has since been recognized as a common complication of diabetes mellitus and other peripheral neuropathic conditions.
The Mechanism of Joint Destruction
The pathophysiology of Charcot neuroarthropathy involves a combination of factors that contribute to joint degeneration. Initially, the loss of sensory feedback leads to repetitive trauma and microtrauma to the joints. Patients may unknowingly engage in activities that place excessive stress on their feet, resulting in fractures, dislocations, and severe joint damage over time.
Inflammation plays a significant role in the progression of Charcot neuroarthropathy. Following the initial trauma, the body’s inflammatory response may exacerbate the condition, leading to increased joint swelling and further damage. While inflammation is a natural part of the healing process, the lack of pain sensation can prevent individuals from modifying their behavior, perpetuating the cycle of injury and inflammation.
Additionally, the mechanical instability that arises from joint destruction can lead to a cascade of complications. As the architecture of the foot changes, the distribution of weight shifts, placing further stress on other joints and tissues. This can lead to the development of secondary deformities, worsening the overall condition and complicating treatment.
Risk Factors for Charcot Neuroarthropathy
While Charcot neuroarthropathy can occur in various patient populations, certain risk factors increase the likelihood of developing the condition. The most significant risk factor is diabetes mellitus, particularly in individuals with poorly controlled blood sugar levels. Diabetic neuropathy is a common complication of diabetes, leading to the sensory deficits that underlie Charcot neuroarthropathy.
Other conditions that can contribute to the development of Charcot neuroarthropathy include:
- Peripheral neuropathy: Conditions such as alcohol abuse, vitamin deficiencies, and certain autoimmune diseases can lead to nerve damage, increasing the risk of Charcot neuroarthropathy.
- Increased foot pressure: Individuals with foot deformities, such as bunions or hammertoes, may be at higher risk due to the abnormal distribution of weight leading to unrecognized injuries.
- Previous trauma: A history of foot injuries or surgical procedures can predispose individuals to Charcot neuroarthropathy, as these factors may compromise the integrity of the joints.
Clinical Presentation and Diagnosis
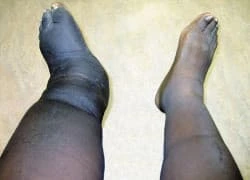
The clinical presentation of Charcot neuroarthropathy can vary widely among individuals, which can complicate the diagnosis. Patients may present with swelling, redness, warmth, and deformity in the affected joints. In the early stages, the condition may resemble an infection or inflammatory arthritis, making it essential for healthcare providers to differentiate between these conditions.
Diagnosis typically involves a combination of clinical evaluation and imaging studies. A thorough history and physical examination are crucial, focusing on the patient’s neuropathic status and any contributing factors. Imaging studies, such as X-rays, MRI, or CT scans, can help assess the extent of joint damage and rule out other conditions.
Early diagnosis is vital in managing Charcot neuroarthropathy effectively. Delayed recognition can lead to irreversible joint destruction and significant disabilities. Therefore, healthcare providers should maintain a high index of suspicion for Charcot neuroarthropathy in at-risk populations, particularly those with diabetes and peripheral neuropathy.
Management and Treatment Strategies
The management of Charcot neuroarthropathy requires a multifaceted approach aimed at preventing further joint destruction and facilitating healing. The primary goals of treatment include reducing weight-bearing stress on the affected joint, managing inflammation, and promoting healing.
1. Offloading
One of the critical components of managing Charcot neuroarthropathy is offloading the affected foot. This can be achieved through the use of specialized footwear, such as a total contact cast or a removable walking boot. These devices help distribute weight evenly across the foot, minimizing stress on the affected joints and allowing for healing.
2. Medication
Anti-inflammatory medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), may be used to manage pain and reduce inflammation in the affected joints. In some cases, corticosteroids may be prescribed to control severe inflammation, although their use should be carefully monitored due to potential side effects.
3. Physical Therapy
Rehabilitation and physical therapy play a vital role in the recovery process. After the acute phase has resolved, physical therapy can help improve strength, flexibility, and range of motion in the affected joints. The therapist may also provide education on proper gait mechanics and strategies to prevent future injuries.
4. Surgical Intervention
In cases where conservative management fails to provide relief or where significant deformities develop, surgical intervention may be necessary. Surgical options can include joint stabilization procedures, realignment of bone structures, or even joint fusion in severe cases. The goal of surgery is to restore function, alleviate pain, and prevent further complications.
5. Continuous Monitoring
Ongoing monitoring and follow-up are crucial in the management of Charcot neuroarthropathy. Regular assessments can help identify any changes in the condition and allow for timely interventions to prevent further joint destruction. Patients should be encouraged to report any new symptoms or changes in their foot condition promptly.
The Importance of Education and Self-Care
Education plays a vital role in the management of Charcot neuroarthropathy. Patients and their caregivers should be informed about the condition, its risk factors, and the importance of regular foot care. Daily foot inspections can help identify any injuries or changes that may require medical attention.
Furthermore, individuals with diabetes should prioritize blood sugar management to reduce the risk of developing neuropathy and, consequently, Charcot neuroarthropathy. Maintaining a healthy lifestyle through proper nutrition, regular exercise, and routine medical check-ups can contribute to better overall foot health.
Conclusion: Raising Awareness of Charcot Neuroarthropathy
Charcot neuroarthropathy represents a complex interplay between nerve damage and joint destruction, with significant implications for affected individuals. Understanding this condition's mechanisms, risk factors, and management strategies is crucial for preventing complications and promoting better outcomes.
By recognizing the signs and symptoms of Charcot neuroarthropathy and prioritizing early intervention, patients can mitigate the risks associated with this debilitating condition. Education, self-care, and collaboration with healthcare providers are essential components of effective management.
For further insights and resources on Charcot neuroarthropathy and other health-related topics, visit Ler Magazine. Empower yourself with knowledge and take proactive steps toward maintaining your health and well-being!









Sign in to leave a comment.