How a Reliable RCM Company Keeps Healthcare Organizations Financially Healthy
Running a healthcare practice today is more challenging than ever. Between patient care, compliance requirements, and endless administrative work, healthcare providers are often stretched thin. Most physicians would rather focus on treating patients than worrying about claim denials, billing errors, or delayed reimbursements.
That’s why Revenue Cycle Management (RCM) companies have become a vital part of modern healthcare operations. They bring order, efficiency, and clarity to the complex financial side of medical practice.
Let’s take a deeper look at how an RCM company functions, why it’s so essential, and how it helps healthcare providers thrive financially while maintaining focus on quality care.
What Does an RCM Company Actually Do?
Revenue Cycle Management (RCM) is the process of tracking the financial journey of a patient — from the time they make an appointment until the healthcare provider receives full payment for the services rendered.
This process sounds simple, but it includes multiple steps that must be executed perfectly. A professional RCM company takes responsibility for every stage of this journey, ensuring smooth revenue flow and minimizing financial disruptions.
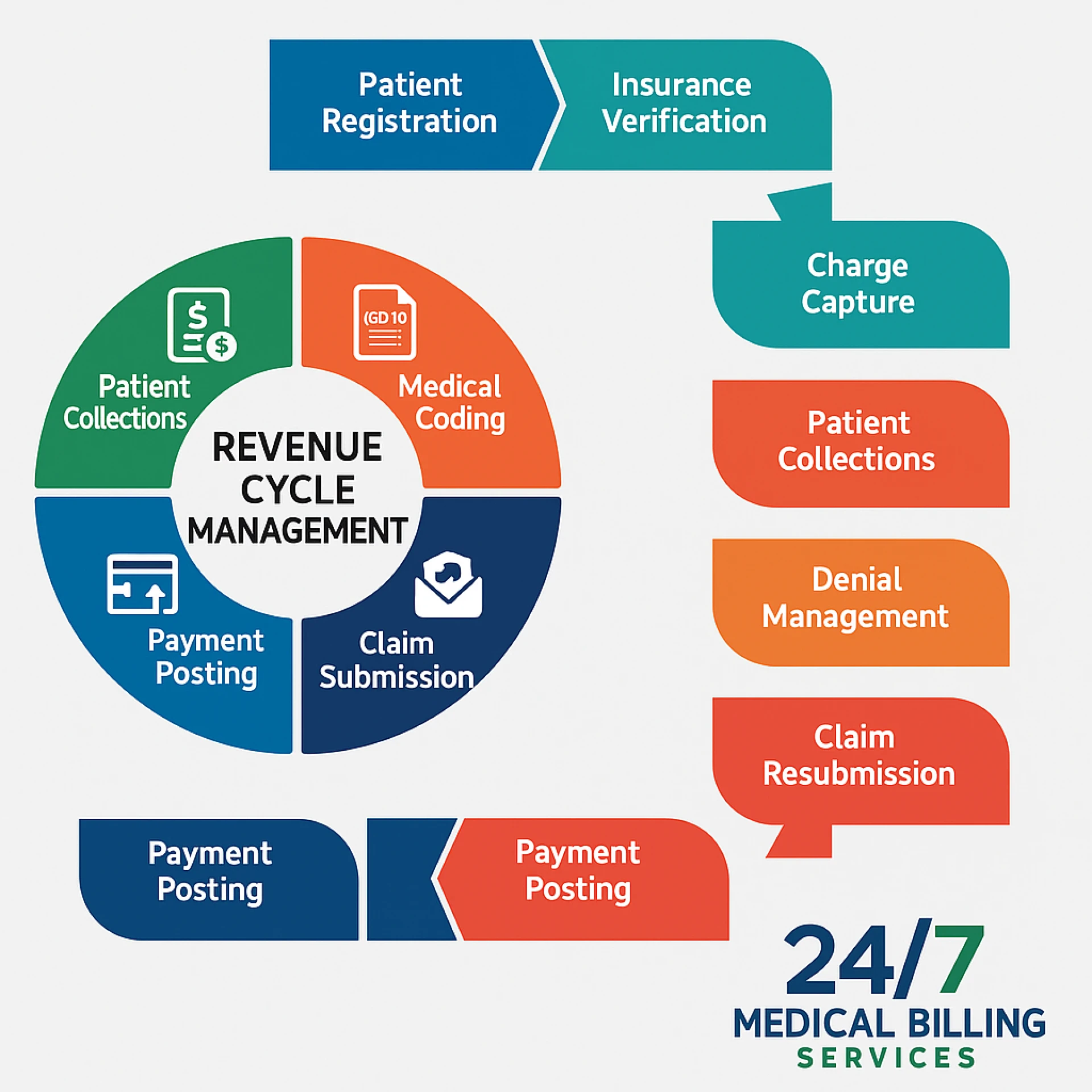
Here’s a step-by-step look at what RCM companies handle:
1. Patient Registration & Insurance Verification
Before an appointment, the RCM team confirms insurance eligibility and benefits. This helps prevent claim denials due to coverage issues.
2. Medical Coding and Billing
After the visit, RCM specialists translate the provider’s notes into accurate medical codes based on standard coding systems such as ICD-10, CPT, and HCPCS.
3. Claim Submission
The coded data is then submitted electronically to insurance companies. A good RCM company ensures that all claims are error-free and meet payer-specific requirements.
4. Payment Posting
Once payments are received, the RCM team records them in the system, matches them with patient accounts, and identifies underpayments or missing amounts.
5. Denial Management and Appeals
If claims are denied or rejected, the RCM specialists find the reason, correct the issue, and resubmit appeals promptly.
6. Patient Billing and Support
The final step is patient billing — generating clear statements and assisting patients with their payment-related questions.
Each stage requires precision and compliance. Even one small error can delay payment or cause revenue leakage. That’s why having a skilled RCM partner is so important.
Why More Healthcare Providers Are Outsourcing to RCM Companies
The healthcare financial system is complicated — thousands of codes, ever-changing payer policies, and strict compliance rules. For most providers, managing all of this in-house is overwhelming and expensive.
Outsourcing to a trusted RCM company offers both financial and operational benefits. Here’s why many medical practices are choosing this route:
1. Better Cash Flow and Faster Payments
RCM companies specialize in reducing claim denials and accelerating reimbursement cycles. They have dedicated teams who monitor each claim, follow up with payers, and ensure that payments are received as quickly as possible.
This consistent cash flow keeps practices financially stable and reduces the stress of waiting on delayed payments.
2. Improved Accuracy and Compliance
Billing and coding errors are among the top causes of revenue loss. RCM professionals undergo continuous training to stay updated with healthcare regulations and coding standards. Their accuracy not only minimizes denials but also protects the provider from compliance penalties.
3. Significant Cost Savings
Maintaining an in-house billing department means hiring staff, buying software, and managing ongoing training. Outsourcing to an RCM company eliminates these expenses. Providers only pay for the services they need, making it a cost-effective option.
4. Data Transparency and Reporting
Modern RCM companies provide detailed analytics on claim performance, denial trends, and payment timelines. These reports give providers a clear picture of their financial health and help them make informed business decisions.
5. More Time for Patient Care
When the financial and administrative side is managed efficiently, doctors and nurses can devote more time to what truly matters — their patients. The entire workflow becomes smoother, and the quality of care improves naturally.
How RCM Companies Are Changing with Technology
Revenue cycle management isn’t what it used to be. The best RCM companies are now tech-driven, using automation, artificial intelligence, and predictive analytics to manage claims faster and more accurately.
For instance:
· Automated claim scrubbing tools identify errors before submission, reducing rejection rates.
· AI-based analytics detect payment trends and forecast potential issues before they become problems.
· Cloud-based dashboards allow providers to see real-time data on revenue, payments, and performance metrics.
By combining human expertise with advanced technology, RCM companies ensure both accuracy and efficiency — a balance that’s essential in today’s healthcare environment.
The Human Side of RCM
While technology plays a huge role, the real strength of an RCM company lies in its people — the billing experts, coders, analysts, and client managers who understand both the technical and emotional sides of healthcare.
They not only handle numbers and claims but also communicate with patients, insurers, and providers in a clear and empathetic manner. Patients appreciate transparent billing, and providers appreciate reliable communication.
This human touch builds trust — something no software can replace.
Key Qualities of a Good RCM Company
Choosing the right RCM partner is a strategic decision. Here are a few qualities that set the best companies apart:
· Experience Across Medical Specialties:
From cardiology and orthopedics to behavioral health and radiology, each specialty has unique billing needs. A good RCM company understands these nuances.
· Commitment to Compliance:
They follow HIPAA regulations and ensure that all patient data is secure and confidential.
· Transparent Processes:
Providers should always know what’s happening with their revenue. A transparent RCM partner shares reports regularly and explains every detail clearly.
· Scalable Services:
Whether you’re a solo practitioner or a large hospital network, the RCM company should scale services according to your needs.
· Proven Track Record:
Client testimonials, case studies, and long-term relationships indicate trust and efficiency.
The Broader Impact of RCM Companies on the Healthcare Industry
An effective RCM company doesn’t just help one practice — it strengthens the entire healthcare ecosystem. When payments are processed correctly, clinics can invest more in advanced equipment, hospitals can hire more staff, and patients can receive better care.
It also reduces the administrative load across the system. Physicians who once spent hours fixing claim errors now spend that time with patients. Financial predictability allows practices to plan ahead confidently.
In short, RCM companies play a silent yet powerful role in keeping healthcare running smoothly.
Real-Life Example: The Power of Efficient RCM
Imagine a small dermatology clinic struggling with frequent claim denials. The staff is overwhelmed, and revenue has started to dip. After partnering with a professional RCM company, the clinic sees results within months:
· Denials drop by 40%
· Payment turnaround time improves by 25%
· Patient satisfaction scores rise because of clearer billing
This transformation shows how strategic RCM support can turn around the financial health of a medical practice.
The Future of Revenue Cycle Management
As the healthcare sector moves toward value-based care and digital transformation, RCM companies are evolving too. The focus is shifting from just “billing management” to “financial performance optimization.”
Future RCM services will likely include:
· Predictive analytics for claim success
· AI-assisted coding to eliminate manual errors
· Integrated payment systems for faster patient transactions
· Real-time financial monitoring through cloud platforms
This evolution means that RCM companies will become long-term strategic partners rather than external vendors.
Conclusion: A Strong Partner for a Stronger Practice
In today’s healthcare environment, financial management is not just about getting paid — it’s about ensuring sustainability and growth. A reliable RCM company helps achieve exactly that.
By streamlining billing, improving claim accuracy, ensuring compliance, and enhancing patient experience, RCM companies free healthcare professionals from financial stress and let them do what they do best — deliver exceptional care.
Whether you’re a small clinic or a large hospital, partnering with a trusted RCM company is no longer optional; it’s a smart move toward stability, efficiency, and long-term success.







Sign in to leave a comment.