In recent years, the healthcare industry has been transformed by a wave of digital innovation but none more powerful than predictive analytics. By using advanced algorithms and real-time data, healthcare providers can now anticipate patient risks, optimise operational workflows, and personalise treatment plans with unprecedented accuracy.
This article explores how predictive analytics in healthcare is reshaping clinical decision-making, improving patient outcomes, and boosting efficiency across the care continuum.
Understanding Predictive Analytics in Healthcare
Predictive analytics applies statistical methods and machine learning to vast datasets to forecast future outcomes. In healthcare, this means using patient demographics, clinical data, and broader health indicators to predict risks—such as hospital readmissions, disease progression, or infection outbreaks—and to guide interventions proactively.
By analyzing historical and real-time inputs, healthcare providers can detect subtle patterns invisible to human judgment and act before complications arise. This shifts care from reactive to anticipatory—and saves time, lives, and resources.
Key Applications and Benefits
1. Early Disease Detection and Management
Predictive models help identify individuals at high risk for conditions like diabetes, cardiovascular disease, or sepsis—even before symptoms appear. This enables targeted preventive interventions and improves long-term health outcomes.
2. Reducing Readmissions
Hospital readmissions are costly and often preventable. Predictive analytics can pinpoint patients most likely to be readmitted—based on clinical, social, and behavioral data—allowing care teams to schedule follow-ups or home health support before problems escalate.
3. Optimizing Resource Allocation
By forecasting patient volumes, predictive models help hospitals allocate staff and equipment more effectively. This is particularly valuable during acute periods like flu seasons or public health emergencies.
4. Personalized Treatment
Instead of one-size-fits-all care, predictive analysis can match patients to treatments that historically yield the best outcomes for their profiles. This includes identifying those most likely to benefit from surgeries, medications, or lifestyle interventions.
5. Public Health Surveillance
Population-level data models allow health authorities to detect disease hotspots, track infection trends, and anticipate outbreaks—empowering timely public health responses and containment efforts.
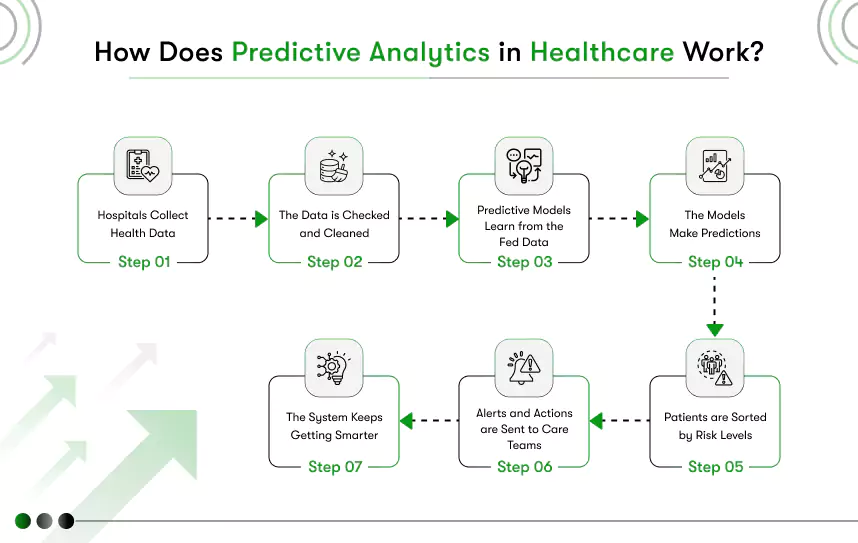
How Predictive Analytics Works in Practice
- Data Collection
- Sources include electronic health records (EHRs), labs, wearable devices, demographic profiles, and even social determinants like socio-economic status or environmental data.
- Data Preparation
- Cleansing data, managing duplicates, and structuring mixed-format data (text, numeric, imaging) is essential before feeding it into predictive models.
- Model Development
- Techniques range from regression analysis to deep neural networks, chosen based on prediction task (e.g., logistic regression for risk classification, time-series forecasting for patient volume).
- Validation & Testing
- Models are tested using historical data and continuously refined to ensure accuracy, fairness, and reduction of bias.
- Deployment
- Integrated into clinical workflows, models trigger alerts—such as “High risk of 30-day readmission”—so clinicians can take proactive action.
- Monitoring & Feedback
- Performance is tracked over time, and models are updated with new outcomes data to maintain clinical relevance.
Real-World Examples
- Sepsis Prediction: Early-warning systems leveraging vital signs and lab results flag at-risk patients hours before clinical symptoms present, enabling timely treatment and reduced mortality.
- Surgical Outcome Forecasting: Models trained on medical histories and procedural data provide tailored survival and complication probabilities, guiding shared decision-making.
- Hospital Capacity Planning: Predictive tools forecast bed occupancy or ICU demand 7–10 days ahead, empowering staff to manage staffing, electives, and resource allocation smoothly.
- Population Health Management: Algorithms identify high-risk cohorts for chronic disease interventions—in areas like diabetes prevention or cardiovascular tracking—streamlining outreach programs.
Challenges and Considerations
- Data Privacy and Security
- Protecting patient privacy is essential. Compliance with HIPAA and GDPR is non-negotiable, and strong data governance must be in place.
- Algorithmic Bias
- Models trained on incomplete or skewed datasets can unintentionally produce biased outcomes. Regular audits and fairness testing are critical.
- Clinician Adoption
- Alert fatigue can erode trust. Predictive tools must be highly accurate, clinically explainable, and seamlessly integrated into existing workflows.
- Interoperability
- Fragmented data systems across departments and providers hinder comprehensive analytics. A centralized or harmonized data infrastructure is needed.
- Regulatory Landscape
- As predictive tools influence clinical decision-making, they may face scrutiny from regulators. Transparent validation and reporting help preempt compliance concerns.
Preparing for the Future
1. Ethical AI Governance
Establish committees that include clinicians, data scientists, and ethicists to oversee development and deployment of predictive models.
2. Explainable AI (XAI)
Ensure models can explain why a certain patient is marked “high risk.” Explainability fosters clinician trust and informed decision-making.
3. Clinically Driven Design
Co-design model alerts with clinicians to align with real-world workflows and reduce alert fatigue.
4. Continuous Monitoring
Track model performance, calibration, and fairness post-deployment to sustain relevance and accuracy.
5. Cross-Institution Collaboration
Shared frameworks and federated learning can enable secure model development using multicentric data—boosting generalizability and performance.
Looking Ahead: AI’s Next Chapter in Healthcare
- Multi-modal Predictive Tools: Integrate imaging, genomics, and lifestyle data to tailor personalized treatment paths.
- Wearable-Driven Models: Live monitoring of vitals and behaviors builds real-time risk profiles for early intervention.
- Virtual Health Assistants: AI agents that interface with models to guide patients post-discharge—suggesting medication adherence or lifestyle actions.
- Clinical Trial Optimization: Dynamic monitoring identifies trial participants at risk of dropout, improving trial efficiency and compliance.
- Population-Scale Forecasting: Predictive models anticipate disease burden across big populations—supporting resource planning and policy design.
Conclusion:
Predictive analytics in healthcare is more than a trend it’s a paradigm shift. The capacity to forecast risk, personalize care, and act preemptively transforms both patient outcomes and healthcare efficiency. As model sophistication and data infrastructure evolve, so too will the possibilities for smart, patient-centered care.
Healthcare organizations ready to adopt these tools today will not only lead in clinical care but also in trust, resilience, and compassion making predictive power a force for good.







Sign in to leave a comment.