Foot drop, a condition characterized by the inability to lift the front part of the foot, can significantly impact an individual's mobility and quality of life. This condition often occurs as a result of nerve damage, muscle weakness, or a combination of both. It can be caused by various factors, including neurological disorders, injury to the nerves, or as a side effect of certain medical conditions, such as stroke, multiple sclerosis, or cerebral palsy. One of the most effective ways to manage foot drop is through physical therapy, which helps to improve strength, flexibility, and coordination.
Understanding the Impact of Foot Drop
Foot drop can manifest in several ways, including dragging the foot, difficulty in lifting the toes while walking, and a high-stepping gait. This condition can make walking tiring, slow, and sometimes dangerous, as it increases the risk of tripping and falling. People with foot drop often need to adapt their daily routines, and they may require assistive devices, such as braces or orthotics, to improve their mobility.
Physical therapy plays a crucial role in managing foot drop by addressing the underlying causes and working to restore functional movement. Through targeted exercises and specialized techniques, physical therapists help individuals regain control over their movements, improving their ability to walk and perform daily activities.
The Role of Physical Therapy in Foot Drop Management
Restoring Strength and Function in the Foot and Ankle
One of the key goals of physical therapy for foot drop management is to strengthen the muscles responsible for lifting the foot and ankle. The dorsiflexor muscles, which control the upward movement of the foot, are often weakened or impaired in individuals with foot drop. Physical therapists develop customized exercise programs that focus on strengthening these muscles and improving overall lower limb strength. These exercises often include:
- Ankle Dorsiflexion Exercises: These exercises involve moving the foot upward against resistance to strengthen the muscles that lift the foot.
- Toe Raises: By raising the toes while keeping the heel on the ground, individuals can target the dorsiflexors and improve their ability to lift the foot during walking.
- Resistance Band Workouts: Using resistance bands, physical therapists can target the muscles in the foot and ankle, helping to build strength in a controlled manner.
Through consistent practice, these exercises can improve muscle function, contributing to better control of foot movement and increased walking stability.
Improving Range of Motion and Flexibility
Another crucial aspect Management of Foot Drop through physical therapy is improving the range of motion and flexibility in the foot and ankle. Tightness in the calf muscles or limited movement in the ankle joint can contribute to the inability to lift the foot properly. Stretching exercises and techniques designed to enhance flexibility help to reduce muscle stiffness and improve overall movement.
Physical therapists often incorporate the following into their sessions:
- Calf Stretches: Stretching the calf muscles helps to improve ankle mobility and reduces tightness in the lower leg, which can impact the ability to lift the foot.
- Ankle Circles: This exercise involves rotating the ankle in circular motions, which enhances flexibility and helps improve joint movement.
- Tendon Stretching: Stretching the tendons in the foot and lower leg can prevent further muscle atrophy and maintain flexibility in the affected area.
By focusing on improving the range of motion, physical therapy helps to restore normal movement patterns and reduces the functional limitations that individuals with foot drop may face.
Enhancing Balance and Coordination
Foot drop can affect an individual's balance and coordination, making it difficult to maintain stability while standing or walking. Physical therapy often includes exercises designed to improve balance and prevent falls. These exercises help individuals regain control over their movements and build confidence when walking.
Common exercises to improve balance and coordination include:
- Standing on One Leg: This exercise helps to strengthen the muscles responsible for maintaining balance and stability.
- Heel-to-Toe Walking: Practicing heel-to-toe walking helps improve coordination and reinforces proper gait mechanics.
- Balance Boards and Stability Exercises: These tools challenge the body’s balance system and help improve ankle and foot stability.
By targeting balance and coordination, physical therapy addresses one of the most challenging aspects of living with foot drop, allowing individuals to walk more confidently and reduce the risk of falls.
Functional Training and Gait Reeducation
In addition to strengthening exercises and balance training, physical therapists work with patients to improve their walking patterns through functional training and gait reeducation. Individuals with foot drop often develop compensatory movement patterns, such as lifting the knee higher while walking to avoid dragging the foot. These abnormal gait patterns can lead to further complications, including joint strain and muscle imbalances.
Physical therapy for gait reeducation focuses on:
- Proper Foot Placement: Teaching individuals to lift their foot fully during walking and place it properly on the ground reduces the risk of tripping and improves walking efficiency.
- Step-Length Training: Encouraging the use of an appropriate step length helps reduce compensatory movements and prevents excessive strain on the hip and knee joints.
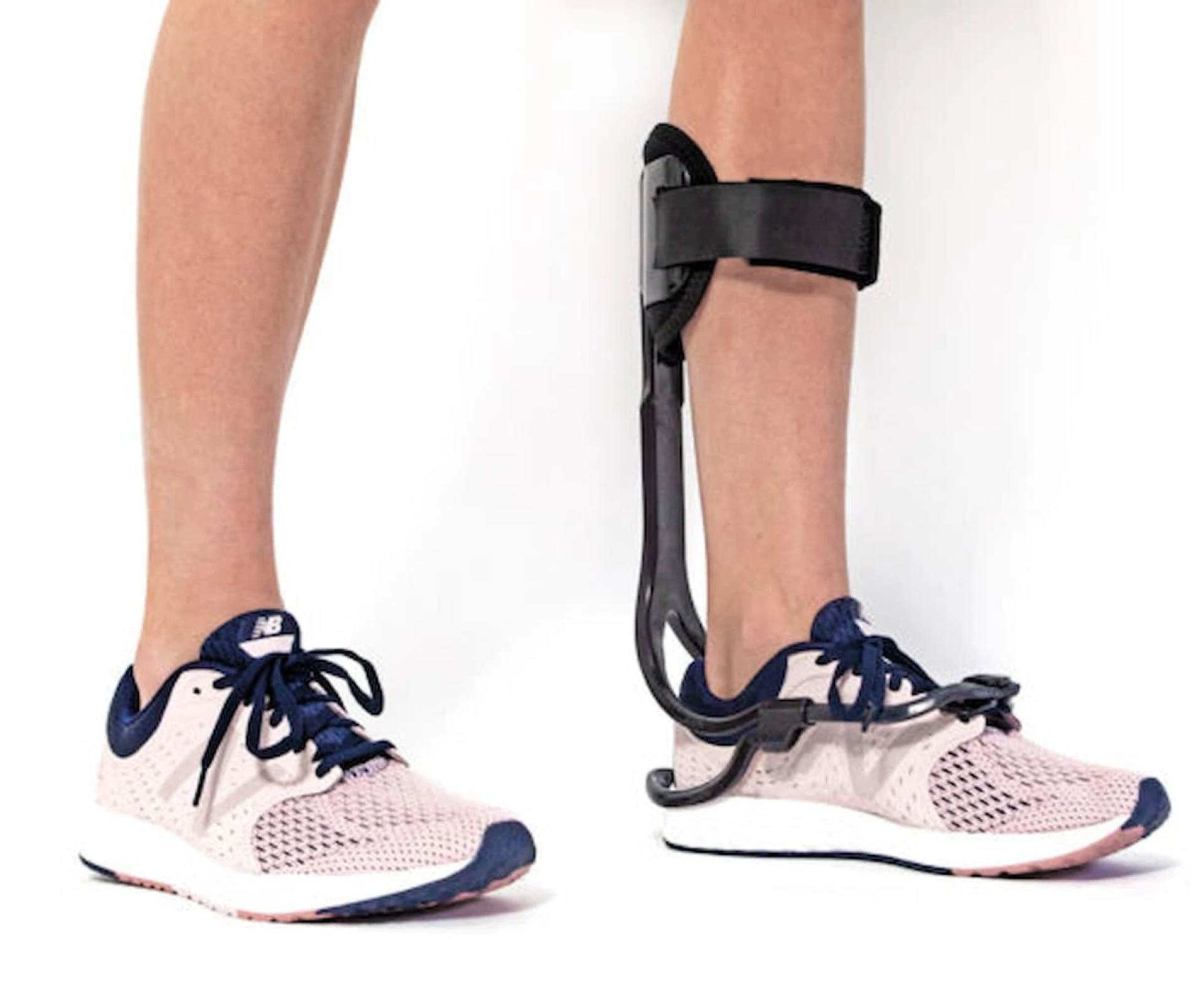
- Gait Training Devices: For individuals with more severe foot drop, physical therapists may incorporate assistive devices such as ankle-foot orthoses (AFOs) to support the foot during walking.
By focusing on proper walking mechanics and adjusting abnormal patterns, physical therapists can help individuals with foot drop improve their gait and mobility.
The Role of Assistive Devices in Foot Drop Management
In some cases, physical therapy may include recommendations for assistive devices to support foot drop management. While physical therapy alone can yield significant improvements, devices like ankle-foot orthoses (AFOs) can provide additional support to the affected foot and ankle. These devices help prevent foot drop during walking and reduce the risk of injury by providing stability and alignment.
Physical therapists work closely with individuals to assess their specific needs and determine the most appropriate devices. They may also teach patients how to properly use these devices to maximize their effectiveness and ensure safety during movement.
Psychological and Emotional Support
Living with foot drop can have a psychological impact, especially if it affects a person’s ability to perform routine tasks or participate in activities they once enjoyed. The emotional toll of dealing with mobility issues and the associated frustration of not being able to walk normally can sometimes be overwhelming.
Physical therapists provide more than just physical support; they also offer emotional encouragement and guidance. By setting achievable goals and celebrating progress, therapists can help individuals with foot drop feel motivated and empowered throughout their rehabilitation journey. This holistic approach to treatment not only addresses the physical symptoms but also promotes mental well-being, helping individuals regain their confidence and independence.
Conclusion
Physical therapy plays a vital role in the management of foot drop. Through targeted exercises, flexibility training, balance improvement, gait reeducation, and emotional support, physical therapists can help individuals regain mobility, prevent further complications, and enhance their quality of life. With a personalized approach to treatment, physical therapy offers hope for those living with foot drop, empowering them to move forward with greater confidence and control over their movements.









Sign in to leave a comment.