PDR proliferative diabetic retinopathy is a severe complication of diabetes mellitus that affects the retina, the light-sensitive layer at the back of the eye. It is characterized by the growth of abnormal blood vessels (neovascularization) on the retina or optic disc, often resulting from prolonged high blood sugar levels that damage retinal blood vessels. These fragile vessels can leak fluid or blood, leading to complications such as vitreous hemorrhage, retinal detachment, or neovascular glaucoma, all of which pose a significant risk of vision loss. As a leading cause of blindness in working-age adults, understanding and managing PDR proliferative diabetic retinopathy is critical. Advances in medical research have introduced innovative treatment options that offer hope for preserving vision and improving outcomes. This article explores the latest treatment options for PDR proliferative diabetic retinopathy, including established therapies, emerging innovations, and the importance of lifestyle management.
Understanding the Progression of PDR Proliferative Diabetic Retinopathy
PDR proliferative diabetic retinopathy represents the advanced stage of diabetic retinopathy, progressing from non-proliferative diabetic retinopathy (NPDR). In NPDR, retinal blood vessels may leak or become blocked, but PDR proliferative diabetic retinopathy is marked by neovascularization triggered by retinal hypoxia (lack of oxygen). These new vessels are prone to rupture, causing complications that can severely impair vision. Symptoms of PDR proliferative diabetic retinopathy include blurred vision, floaters, dark spots, tunnel vision, and sudden vision loss. Often, symptoms may not appear until the condition is advanced, underscoring the importance of regular eye exams for early detection.
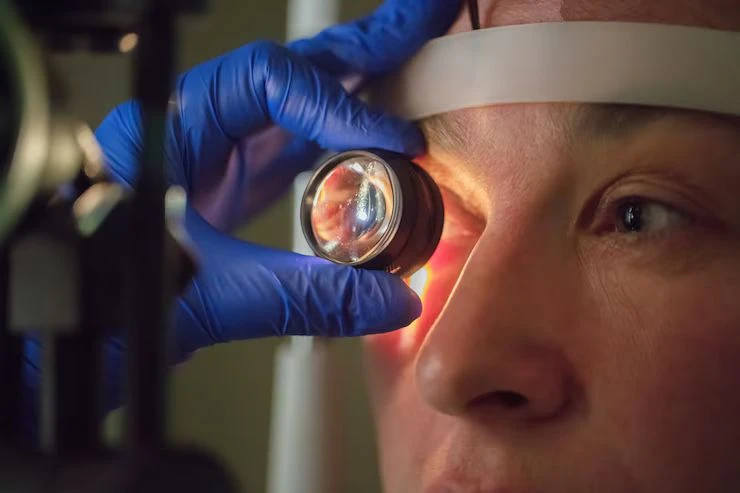
Diagnosis of PDR proliferative diabetic retinopathy involves comprehensive eye examinations, including visual acuity testing, pupil dilation, and imaging techniques such as optical coherence tomography (OCT) and fluorescein angiography. These tests allow ophthalmologists to assess retinal damage, detect abnormal blood vessels, and determine the severity of the condition. Early diagnosis is crucial for timely intervention to prevent irreversible vision loss.
Established Treatment Options for PDR Proliferative Diabetic Retinopathy
The management of PDR proliferative diabetic retinopathy has evolved significantly, with several established treatments proven effective in stabilizing the condition and preventing further vision loss. These include laser therapy, anti-VEGF injections, and surgical interventions.
Panretinal Photocoagulation (PRP)
Panretinal photocoagulation (PRP) has been the cornerstone treatment for PDR proliferative diabetic retinopathy for over four decades. This laser therapy involves creating small burns in the peripheral retina to reduce the growth of abnormal blood vessels. By targeting areas of retinal ischemia, PRP decreases the production of vascular endothelial growth factor (VEGF), a protein that promotes neovascularization. Studies, such as those from the Diabetic Retinopathy Study (1976), have shown that PRP can reduce the risk of severe vision loss by up to 50%. However, PRP may cause side effects, including reduced peripheral vision, decreased night vision, and potential worsening of diabetic macular edema (DME). Despite these limitations, PRP remains a highly effective option, particularly for patients with high-risk PDR proliferative diabetic retinopathy.
Anti-VEGF Injections
Anti-VEGF (vascular endothelial growth factor) injections have revolutionized the treatment of PDR proliferative diabetic retinopathy. Medications such as ranibizumab (Lucentis), aflibercept (Eylea), and bevacizumab (Avastin, used off-label) block VEGF, inhibiting the growth of abnormal blood vessels. These injections are administered directly into the vitreous of the eye and are particularly effective in cases with vitreous hemorrhage or coexisting diabetic macular edema. Clinical trials, such as the DRCR Network’s Protocol S, have demonstrated that ranibizumab is non-inferior to PRP, offering better visual acuity and less visual field loss. However, anti-VEGF therapy requires frequent injections, typically monthly, which can be burdensome for patients. The introduction of next-generation anti-VEGF agents, such as aflibercept 8 mg and faricimab, allows for extended dosing intervals (up to 12–16 weeks), improving patient compliance.
Vitrectomy
In advanced cases of PDR proliferative diabetic retinopathy, where complications like non-clearing vitreous hemorrhage or tractional retinal detachment occur, vitrectomy may be necessary. This surgical procedure involves removing the vitreous gel, blood, or scar tissue from the eye to restore vision and prevent further retinal damage. Vitrectomy is particularly effective for patients with persistent bleeding or retinal detachment threatening the macula. The DRCR Network’s Protocol AB showed that vitrectomy provides quicker visual recovery compared to anti-VEGF alone, although outcomes may be similar in the long term. While vitrectomy is a powerful tool, it carries risks such as infection, cataract formation, or increased intraocular pressure, necessitating careful patient selection.
Emerging Innovations in PDR Proliferative Diabetic Retinopathy Treatment
Recent advancements in medical technology and research have introduced promising new approaches to managing PDR proliferative diabetic retinopathy. These innovations aim to enhance efficacy, reduce side effects, and improve patient outcomes.
Advanced Laser Technologies
Traditional PRP, while effective, can cause thermal damage to retinal tissue, leading to side effects like reduced contrast sensitivity and peripheral vision loss. New laser modalities, such as pattern scanning laser (e.g., Pascal laser) and navigated laser photocoagulation (Navilas), offer more precise and less invasive treatments. The Pascal laser uses shorter pulse durations to minimize heat diffusion, reducing damage to surrounding tissues and patient discomfort. Navilas integrates fundus imaging with laser delivery, allowing for precise targeting of ischemic areas with improved reproducibility. These technologies have shown promise in reducing the progression of diabetic macular edema and inflammatory cytokine levels compared to conventional lasers.
Subthreshold Diode Micropulse Laser
Subthreshold diode micropulse (SDM) laser therapy is an emerging non-destructive approach that stimulates retinal pigment epithelium without causing permanent retinal damage. By delivering energy in short micropulses, SDM minimizes heat buildup, preserving retinal tissue while reducing VEGF production. A retrospective study reported that SDM PRP had comparable outcomes to conventional PRP, with a lower incidence of vitreous hemorrhage (12.5% over one year). While further randomized controlled trials are needed, SDM represents a promising alternative for patients seeking less invasive options.
Combination Therapies
Combining PRP with anti-VEGF injections has emerged as a promising strategy for managing complex cases of PDR proliferative diabetic retinopathy, particularly those with coexisting diabetic macular edema. This approach leverages the rapid neovascular regression induced by anti-VEGF agents and the long-term stability provided by PRP. Studies suggest that combination therapy can improve visual outcomes and reduce the frequency of anti-VEGF injections, making it a viable option for patients with unreliable follow-up.
Artificial Intelligence in Diagnosis and Management
Artificial intelligence (AI) is transforming the diagnosis and management of PDR proliferative diabetic retinopathy. AI algorithms can analyze retinal images to detect early signs of diabetic retinopathy, predict disease progression, and guide treatment decisions. By improving screening accessibility and accuracy, AI has the potential to enhance early intervention, particularly in underserved areas where access to ophthalmologists is limited.
Lifestyle and Systemic Management
While medical and surgical interventions are critical, lifestyle modifications play a vital role in managing PDR proliferative diabetic retinopathy. Maintaining stable blood sugar levels through diet, exercise, and medication adherence is essential to prevent further retinal damage. A diet rich in antioxidants, such as leafy greens and omega-3-rich fish, can support retinal health. Controlling blood pressure and cholesterol levels also reduces the risk of vascular complications. Quitting smoking and engaging in regular physical activity further contribute to overall eye health. Patients should work closely with their healthcare team to optimize diabetes management and undergo regular eye exams to monitor for progression.
Challenges and Considerations
Despite advancements, challenges remain in the management of PDR proliferative diabetic retinopathy. Patient compliance with follow-up visits and treatment regimens is a significant barrier, as highlighted by studies showing that up to 50% of patients may be lost to follow-up for six months or more. This increases the risk of complications like tractional retinal detachment. Additionally, the economic burden of treatments, particularly anti-VEGF injections and surgical procedures, can be substantial. Access to preventive care and early intervention is critical to mitigating these costs and improving outcomes.
Future Directions
The future of PDR proliferative diabetic retinopathy treatment lies in continued innovation and personalized medicine. Ongoing research into gene therapies, novel anti-VEGF agents, and minimally invasive laser techniques holds promise for more effective and less burdensome treatments. Additionally, addressing social determinants of health, such as access to care and transportation, will be crucial for improving patient outcomes. Collaborative efforts between researchers, clinicians, and patients will drive progress in combating this vision-threatening condition.
Conclusion
PDR proliferative diabetic retinopathy remains a significant challenge for individuals with diabetes, but recent advancements in treatment offer hope for preserving vision and improving quality of life. Established therapies like PRP, anti-VEGF injections, and vitrectomy, combined with emerging innovations such as advanced laser technologies, sustained-release implants, and AI-driven diagnostics, provide a comprehensive approach to management. By integrating medical interventions with lifestyle modifications and regular monitoring, patients can effectively manage PDR proliferative diabetic retinopathy and reduce the risk of vision loss. Early detection, timely treatment, and a proactive approach to diabetes care are essential for protecting vision and maintaining independence.







Sign in to leave a comment.