There is no "silver bullet" in determining the success rate of EECP treatment. It is a combination of patient-related outcomes, measurable tests, correct indication, and reproducible application. This article will describe what clinicians and patients measure, what trials reveal about how often people are helped, which variables alter the results, and a common-sense approach you can use when you study reported success rates of EECP treatment.
What is “success” for EECP anyway?
The success is the result of an objective change and relevant symptom relief. Clinical utility outcomes include: reduced angina, decreased number of short-acting nitrate doses, longer treadmill or 6-minute walk distance, and higher patient-reported quality-of-life measures. All programs claiming panecea, in my opinion, should offer some objective pre-/post-data, not just testimonials.
What do the trials and registries report as the success rate?
Most meta-analyses and registries indicate that the vast majority of treated patients experience symptom improvement. Published grouping data and structured reviews consistently report that 60–85% of patients experience at least 1-class angina improvement or a quantifiable functional improvement after completion of an average EECP regimen. Controlled and randomized trials show some improvements in angina frequency and exercise capacity in particular patients, but hard endpoints such as reduction of mortality are not established. Read those numbers as symptomatic-response rates, and not as cures for fully blocked arteries.
Who is most likely to have a good result?
Patients with chronic stable refractory angina who have maximized and are not candidates for further revascularization tend to do best. Patients with typical ischemic symptoms, whose exercise testing capacity is preserved and who are adherent to the full course of treatment, do best. EECP is not indicated for acute coronary syndromes, recent MI, or unstable patients. Coverage and practice guidelines also restrict appropriate indications to chronic, refractory cases.
How is a “course” defined and why does it matter?
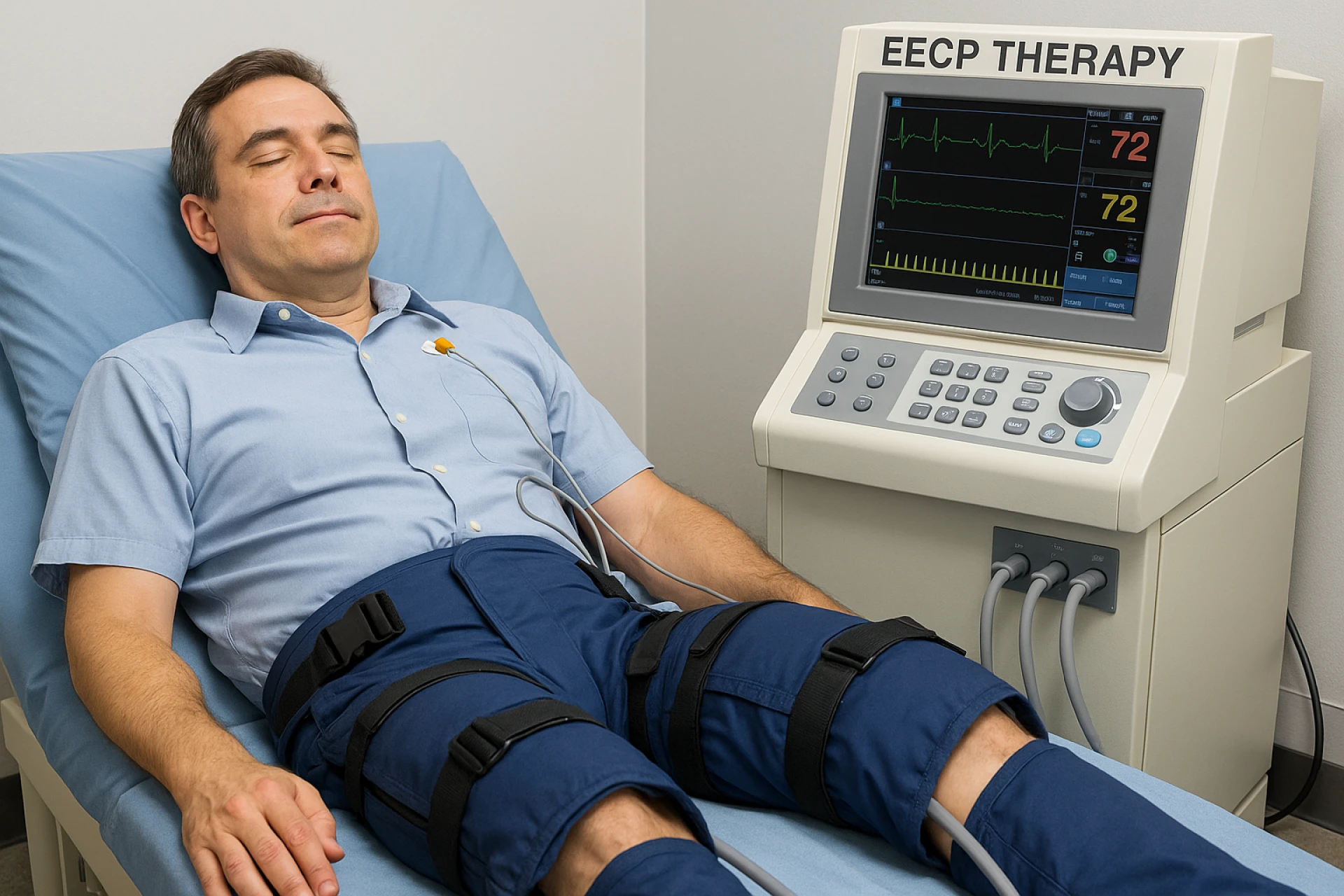
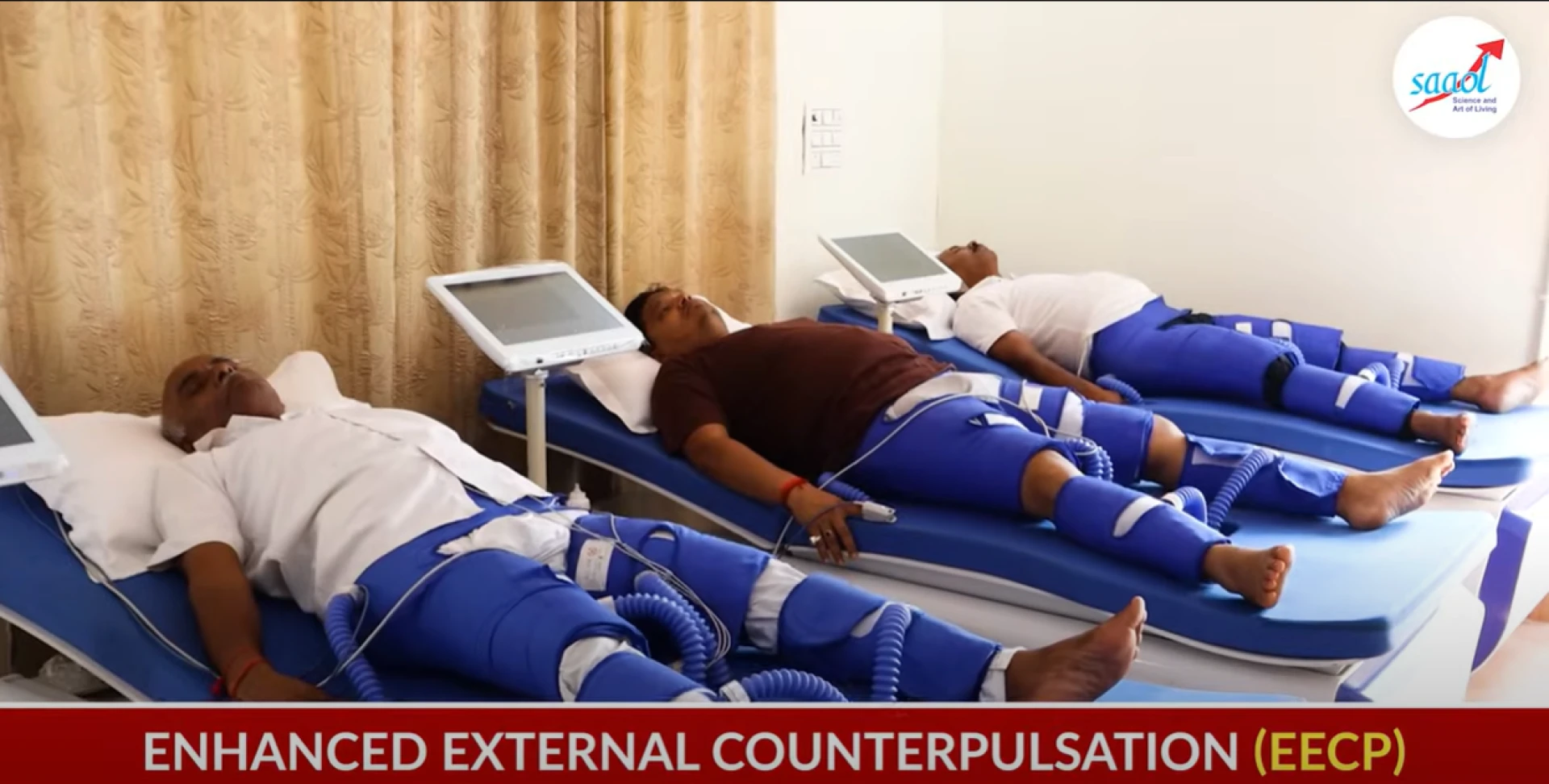
A typical course of EECP treatment is 40 one-hour sessions, typically once a day over six to seven weeks. Evidence of benefit hinges on taking a full and well-supervised course. Incomplete and inadequate therapy also decreases the chance of measurable benefit.
How durable are the benefits of EECP Treatment?
Durability varies. Some observational series and longer follow-ups demonstrate months to years of durable benefit for a significant proportion of patients. The meta-analyses indicate that some patients will continue to have a reduction in angina and improved function up to 3–5 years however results are heterogeneous. Variable outcomes can be anticipated based on how well underlying risk factors, medications, and lifestyle are maximized following EECP.
What factors increase or decrease the success rates of EECP Treatment?
- Patient selection. Strict selection increases success. Treating everyone reduces the apparent rate of success.
- Protocol fidelity. Completing 40 monitored sessions matters. Shortened or unsupervised courses underperform.
- Device and staff expertise. Either well-maintained machines or trained personnel minimize complications and achieve the desired hemodynamic support.
- Baseline disease and comorbidities. Moderately advanced peripheral vascular disease, uncontrolled arrhythmias, limit eligibility and benefit.
- Follow-up care. Success is longer-lasting when EECP is combined with optimal medical therapy, secondary prevention (lifestyle modifications), and risk factor management.
What does “success” not mean?
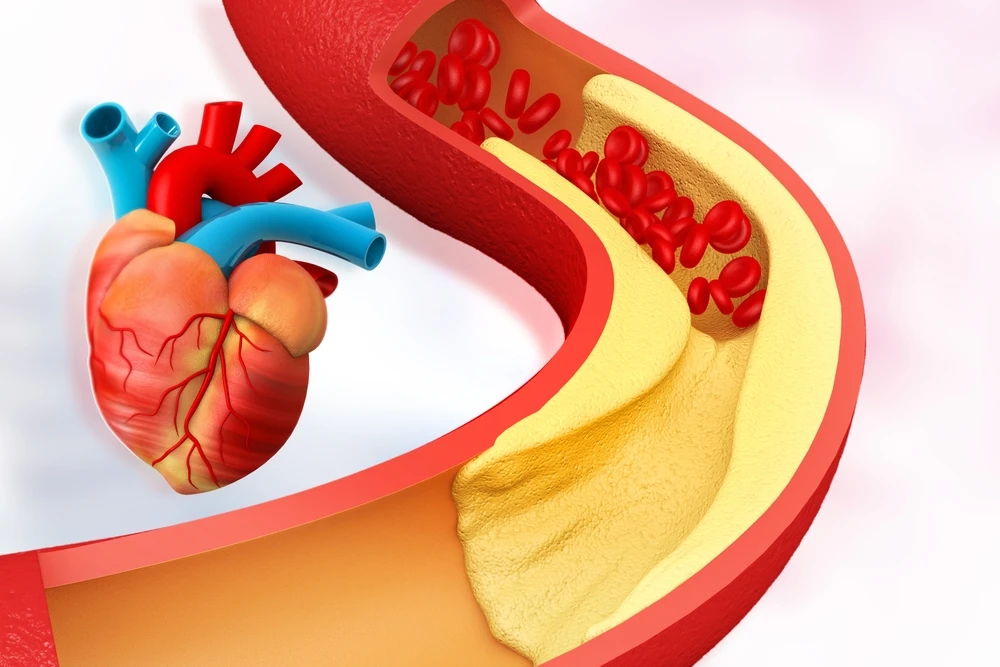
Of course, success in reported series implies symptomatic relief and increased exercise tolerance. It’s not that EECP opens closed arteries as do bypass surgery or angioplasty. Those claims that EECP “removes blockages” are simply a misrepresentation. The treatment intends to increase perfusion, restore endothelial function, and induce collateralization. (natural bypass)
How should clinics report their success rate of EECP Treatment so patients can trust the number?
Trustworthy reporting includes: baseline and post-treatment objective metrics (CCS class, treadmill or 6MWT, nitrate use), the proportion of patients achieving predefined targets, adverse event rates, and median follow-up duration. Aggregate statistics are more useful than selective testimonials. Clinics that publish audited outcomes or participate in registries provide the strongest evidence of program quality.
Practical questions patients have — brief answers
Q: What are my chances of feeling better?
A: Many studies indicate that a majority of people have symptom relief. Anticipate symptomatic improvement in many, but nothing triumphant.
Q: How quickly can I expect change to happen?
A: Some see results in 2–3 weeks. Greatest point gain is made upon course completion.
Q: Are repeat courses needed?
A: Some patients have a second set of treatments if symptoms return. The degree of durability is dependent on the extent of control of the underlying disease.
A compact checklist to maximize your chance of a good outcome
- Obtain a recent cardiology review and objective ischemia testing.
- Choose centers that document baseline and post-treatment metrics.
- Confirm the program uses a 40-session standard and continuous ECG monitoring.
- Ask for aggregated program outcomes and staff credentials.
- Pair EECP with optimized meds, rehab, and risk-factor control.
Bottom line
The success rate of EECP treatment is best read as a symptomatic-response rate in well-selected patients who complete a full, monitored course. High-quality evidence and registries show that a majority of eligible patients achieve meaningful relief in angina and improved exercise capacity. Long-term hard-outcome data are less consistent. The difference between a good and a mediocre reported success rate is selection, protocol fidelity, outcome transparency, and follow-up care. Ask clinics for objective before/after data, not only testimonials, before you commit time and money.







Sign in to leave a comment.